4 results
Infection prevention and control perspective and practices among healthcare workers in Bangladesh: A multicenter cross section
- Md. Golam Dostogir Harun, Shariful Amin Sumon, Aninda Rahman, Md Mahabub Ul Anwar, Md. Saiful Islam
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s74-s75
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Infection prevention and control (IPC) is a critical feature of preventing the spread of healthcare-associated infections (HAIs) in hospitals. IPC practices are particularly important in resource-constrained and crowded hospital settings. The successful implementation of infection prevention measures depends on healthcare worker (HCW) knowledge of, attitude toward, and practice (KAP) of IPC. In this project, we assessed the KAP of HCWs and identified factors associated with IPC compliance at tertiary-care hospitals in Bangladesh. Methods: From September 2020 to January 2021, we conducted this hospital-based cross-sectional assessment at 11 tertiary-care hospitals. A semistructured questionnaire was used to conduct face-to-face interviews with physicians, nurses, and cleaning staff who were directly involved in patient care. Based on >75% of the total score, each KAP component was divided into adequate knowledge, favorable attitude, and safe practice. We performed descriptive analysis and multivariate logistic regression to determine the KAP score and associated factors influencing IPC compliance in hospital settings. Results: In total, 1,728 HCWs were interviewed; 76.8% of the participants had adequate knowledge on IPC and 54.6% reported safe practices. However, only 16.2% of HCWs had a favorable attitude toward IPC. Among the 3 HCW groups, nurses had the highest KAP scores (76.07±12.7) followed by physicians (69.8±16.2), and cleaning staff (34.4±27.3). Only 29.2% of HCWs reported having received IPC training, and they cited heavy workload as a barrier to IPC guideline adherence. HCWs having adequate knowledge showed 9 times higher odds of safe IPC practice (AOR, 9.36; 95% CI, 5.47–16.04). HCWs who had a favorable attitude toward IPC were 16 times as likely to perform safe practice toward IPC activities (AOR, 15.5; 95% CI, 10.27–23.42). Conclusions: Knowledge of safe practices and having a favorable attitude toward IPC are key components of a successful IPC program. Significant improvements are required among all levels of HCWs in Bangladesh tertiary-care hospitals, especially cleaning staff. Educational interventions to train on IPC guidelines, plus monitoring, could improve HCW safe practices.
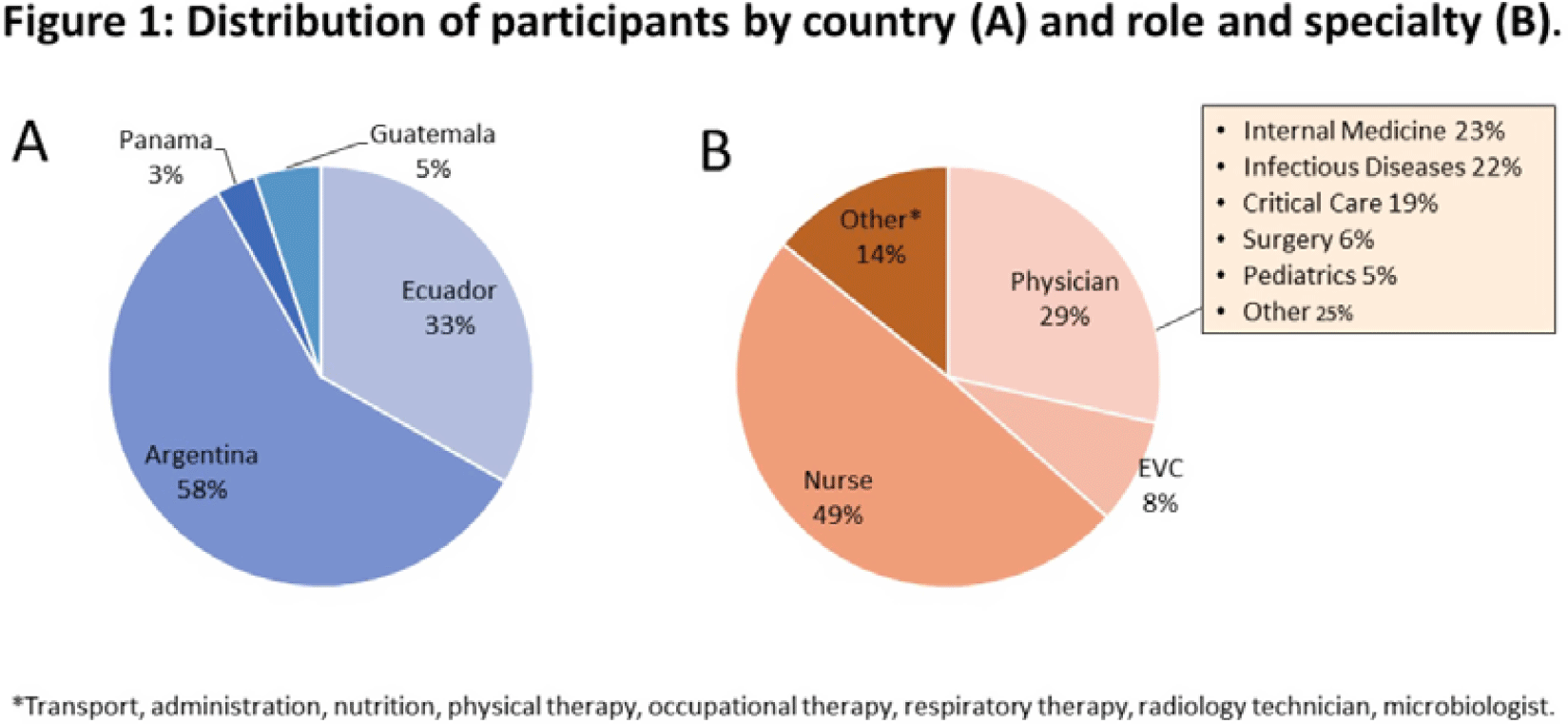
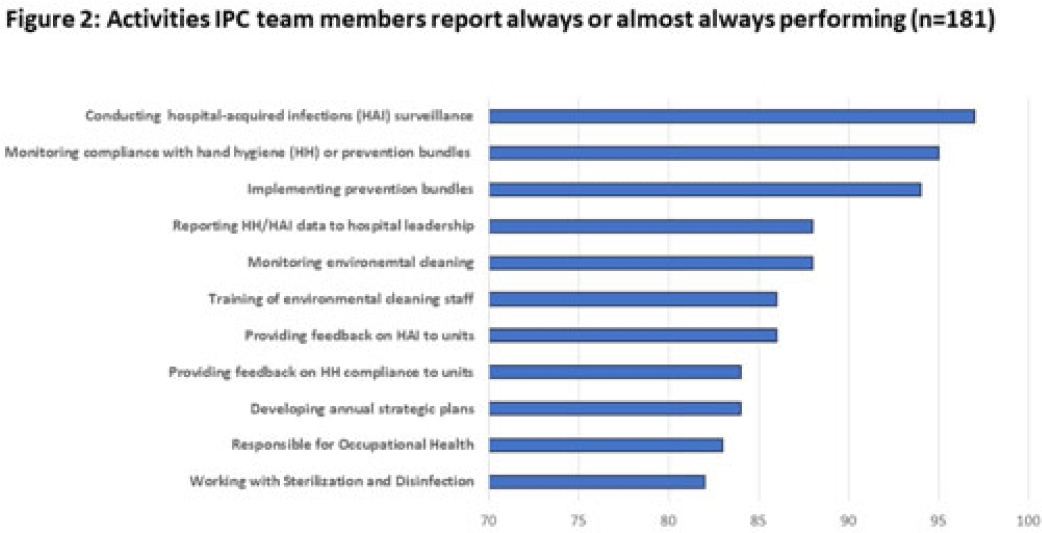
Disclosures: None
Perceptions toward and practices regarding antibiotic stewardship and use among physicians at tertiary-care public hospitals in Bangladesh
- Shariful Amin Sumon, Saiful Islam, Golam Dostogir Harun
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s1
-
- Article
-
- You have access Access
- Open access
- Export citation
-
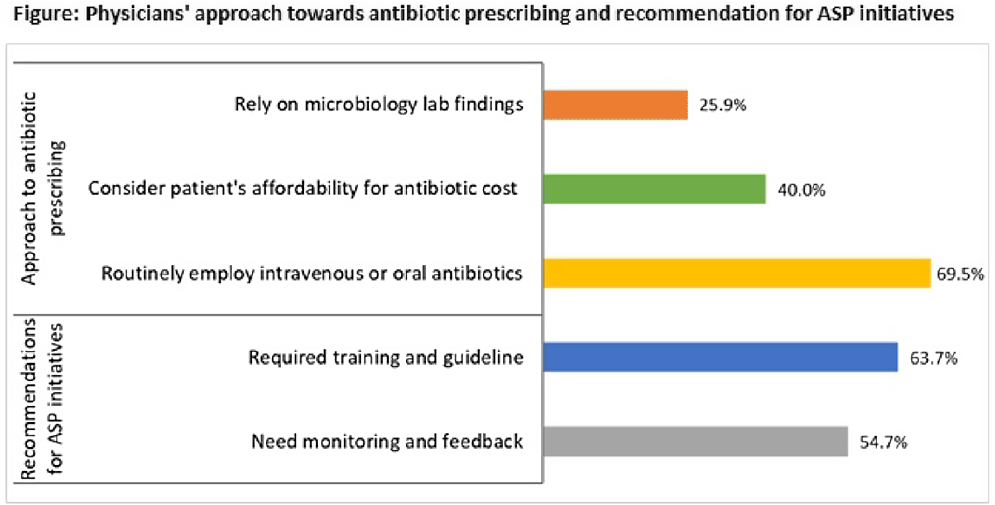
Background: The emergence of antimicrobial resistance (AMR) is affecting public health management in developing countries, including Bangladesh. Irrational and inappropriate use of antibiotics in healthcare settings has led to widespread drug resistance. To optimize antimicrobial usage to combat AMR and enhance infection treatment, the competence of healthcare workers in antibiotic prescribing is indispensable. We sought to determine the perceptions about antimicrobial resistance, antibiotic stewardship programs (ASPs), and antibiotic prescribing approaches among physicians at tertiary-care public hospitals in Bangladesh. Methods: From September to December 2020, we conducted a mixed-methods study in 9 tertiary-care public hospitals. Using a self-administered, semistructured questionnaire, we collected data on antibiotic stewardship and prescribing practices from 452 on-duty physicians. In addition, we conducted 16 key-informant interviews to explore AMR perceptions and determinants. Results: Only 43.8% of physicians were aware of the ASP, and none of the hospitals had any ASP initiative in place. Most of the participants (70.6%) recommended tailored training and antibiotic prescribing guidelines (63.7%) for effective ASP initiatives. More than half of the physicians (54.7%) preferred to receive regular monitoring and feedback on their routine antibiotic prescriptions from the stewardship program. In terms of the antibiotic prescribing approach, only 25.9% of physicians relied on microbiology lab findings, whereas 69.5% routinely employed oral or intravenous antibiotics. Also, 40.0% of physicians considered the patient’s ability to afford the antibiotic cost when recommending antibiotics. The qualitative investigation identified the use of broad-spectrum antibiotics, absence of guidelines, and inadequate laboratory support as factors contributing to AMR in the healthcare setting. Self-medication, over-the-counter dispensing, and patients’ economic instability to complete the dosage were also attributed to the irrational use of antibiotics. As a priority step, physicians advocated for intensive training on antibiotic advising, mass awareness campaigns on safe antibiotic usage and dispensing, and a restriction on the widespread sale of antibiotics from pharmacies. Conclusions: Despite favorable perceptions, the fundamental understanding of physicians regarding ASPs and rational prescribing of antibiotics needs to be improved through context-specific educational interventions and capacity building. In addition, a coherent and comprehensive policy is required for the development and implementation of antibiotic usage guidelines along with integrated ASP initiatives to combat AMR.
Funding: None
Disclosures: None
Compliance and constraints of hand hygiene among healthcare workers in Bangladesh
- Md. Golam Dostogir Harun, Shariful Amin Sumon, Tahrima Mohsin Mohona, Md. Zakiul Hassan, Aninda Rahman, Syed Abul Hassan Md Abdullah, Md. Saiful Islam, Ashley Styczynski
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s46-s47
-
- Article
-
- You have access Access
- Open access
- Export citation
-
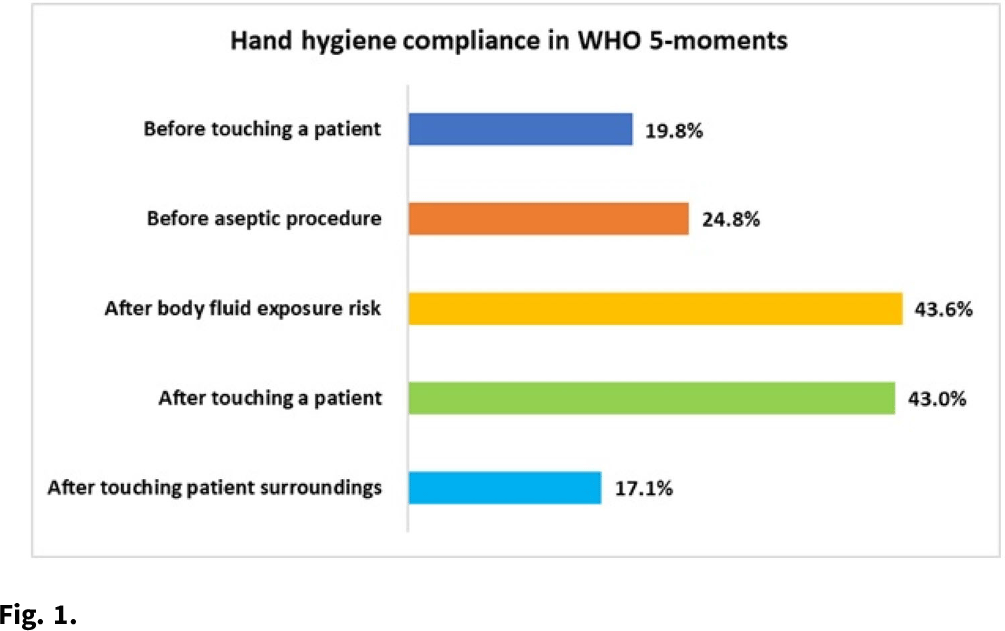
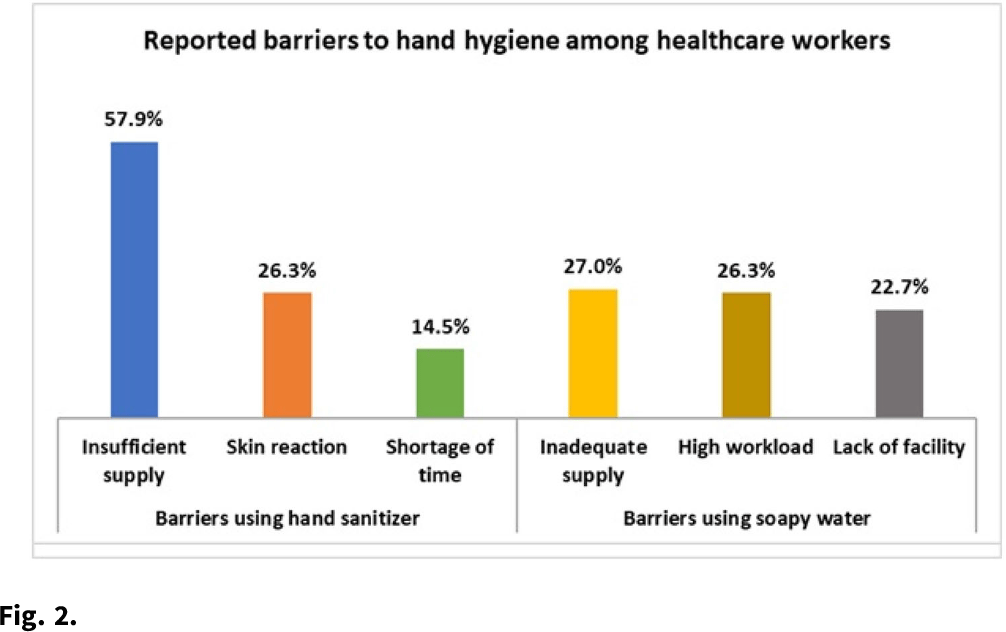
Background: Hand hygiene (HH) is a core element of patient safety and the single most essential strategy for preventing healthcare-associated infections (HAIs). Adherence to HH among healthcare workers (HCWs) varies greatly depending on a range of factors, including risk perceptions, institutional culture, auditing mechanisms, and availability of HH supplies. We observed HH compliance among HCWs to determine the factors influencing practices in tertiary healthcare facilities in Bangladesh. Methods: During September 2020–February 2021, we conducted nonparticipatory observations at 11 tertiary-care hospitals in Bangladesh using the WHO “Five Moments for Hand Hygiene” tool to record compliance among physicians, nurses, and cleaning staff. We also performed semistructured interviews to determine the key barriers to complying with hand hygiene. Furthermore, we noted the presence, location, and functionality of existing HH stations within each hospital ward. Results: We observed 14,668 HH opportunities among HCWs. The overall HH compliance was 25.3%, and compliance differed significantly by professional category (P < .001). Physicians had the highest HH compliance at 28.5% (2,264 of 7,930), followed by nurses at 25.4% (1,272 of 5,008). Cleaning staff had the lowest rates of HH at 9.9% (171 of 3,221). HCWs of public hospitals had significantly higher odds of complying with HH practices than those in private hospitals (27.4% vs 17.9%; aOR, 1.73; 95% CI, 1.55–1.93; P < .001). HH compliance also varied by WHO Five Moments indicators. HCWs were 3 times more likely to perform HH ‘after touching a patient’ than ‘before touching patient’ (aOR, 3.36; 95% CI, 2.90–3.90; P < .001). Common barriers to using hand sanitizer were insufficient supply (57.9%), skin reaction (26.3%), shortage of time (14.5%), and lack of awareness (11.9%). Regarding handwashing with soap, inadequate supplies (27.0%), high workload (26.3%), and lack of facilities (22.7%) were the key factors for low adherence. The HH infrastructure observation in 82 wards showed that running water and soap were available in 168 (86.2%) of 195 HCW-designated basins, compared to 51 (35.9%) of 142 for the patient- and attendant-assigned basins. Handwashing posters were found in only 44 (13.1%) of 337 basin surroundings, and no hand drying supplies were observed for patients or attendants. Conclusions: Hand hygiene compliance among HCWs fall significantly short of the standard for safe patient care. Inadequate HH supplies in a resource-constrained setting like Bangladesh demonstrates a lack of leadership in prioritizing, promoting, and investing in infection prevention and control. The findings of this study might help to motivate and design interventions for HH compliance, which will help reduce HAIs in the hospital setting.
Funding: None
Disclosures: None
Parental Knowledge, Attitudes, and Practices Regarding Antibiotic Use: A Cross-Sectional Study in Bangladesh
- Golam Dostogir Harun MD, Romel Haider, Imdadul Haque MD, Alauddin Chowdhury, ABM, Saiful Islam MD
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s342
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Antibiotics play a vital role in reducing the morbidity and mortality associated with common infectious among children aged <5 years. Objective: We assessed the parental knowledge, attitudes, and practices regarding antibiotic use among a low-income urban population in Bangladesh. Methods: A cross-sectional study was conducted among the parents of 516 low-income urban children aged <5 years in Bangladesh from February 2018 to April 2019. A semi-structured questionnaire was developed and administrated to explore parental knowledge, attitudes, and practice regarding antibiotic use. A logistic regression analysis and Spearman rank-order correlation was used to compare and evaluate possible associations regarding parental KAP on antibiotic use. Results: The mean age of the participants was 26.65 years (SD, 6.38) and average monthly income was US$195.00. Most respondents (437 of 516) were women. One-third of the participants had no formal education, and 64% had only 5 years of education. We categorized the knowledge, attitudes, and practice regarding antibiotic use into 3 categories: poor, moderate, and good. More than half (52%) of these parents had poor knowledge of antibiotic use, and 32% had moderate knowledge of antibiotic use. Overall, 55% of parental attitudes were moderate and 70% of antibiotic practices were moderate. However, only 16% respondents had good knowledge, 14% had good attitudes, and 14% had good practices regarding antibiotic use for their children. The study revealed that 41% of parents thought that their child could be treated with antibiotics without advice from a qualified doctor, and 71% of parents thought that a child with flu-like symptoms got better faster if antibiotics were used. Also, 54% thought that the antibiotics could be stopped as soon as the symptoms disappeared. In this study, only 40% of parents completed the full dose of antibiotics. Monthly family income (P = .005), father’s profession (P = .003), and parents’ education were significantly associated with antibiotic use to treat the child. Conclusions: Most participants’ knowledge, attitude, and practices regarding rational antibiotic usage was very poor. Awareness campaigns and implementation of education on how to purchase, use, and sell antibiotics is crucial to optimum the use of antibiotics in Bangladesh.
Funding: None
Disclosures: None








